Introduction
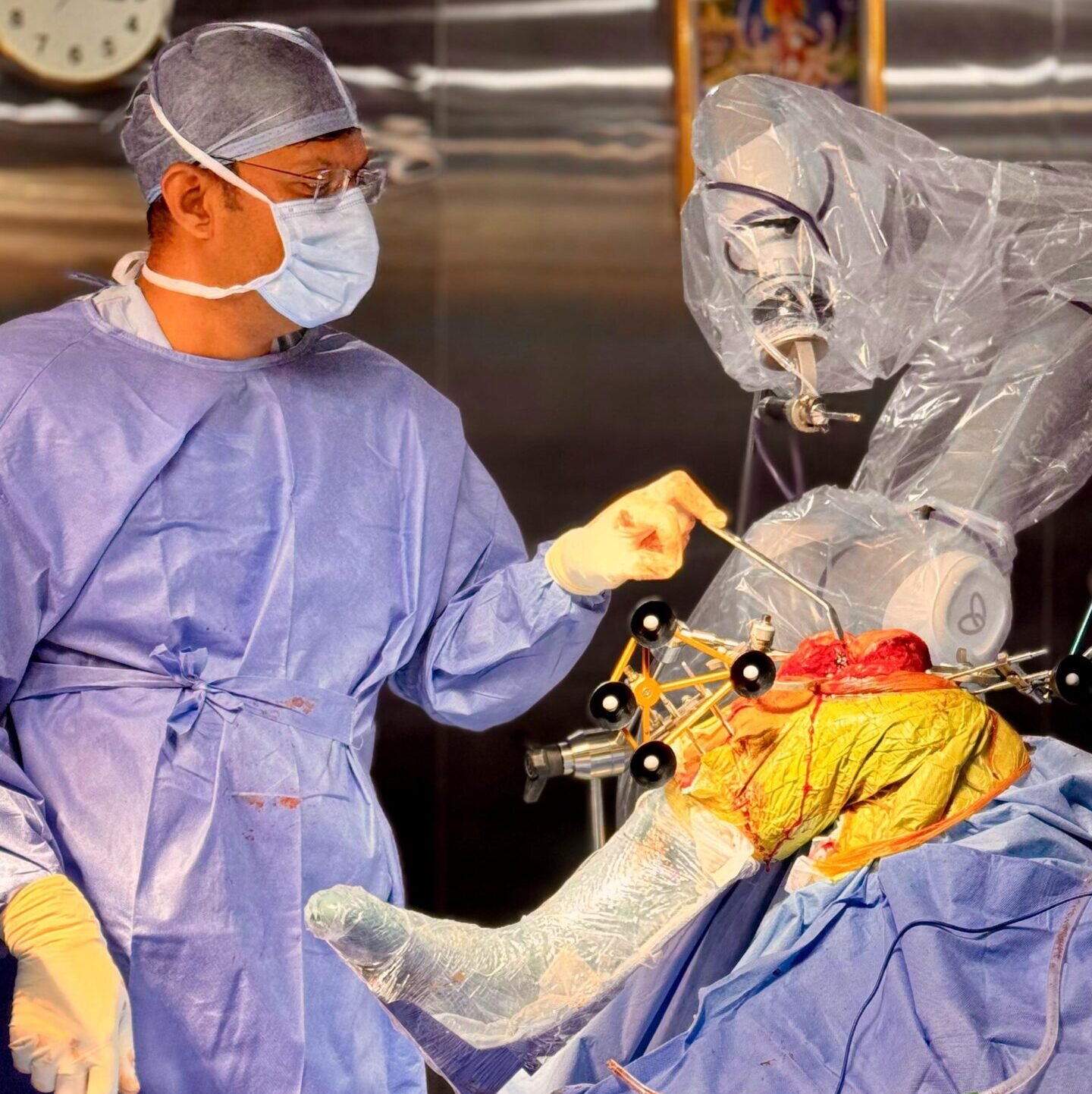
Total knee replacement (TKR) is a major orthopedic procedure requiring a structured rehabilitation program. Success depends not just on the surgery itself, but on your commitment to recovery. This comprehensive guide outlines what to expect and how to optimize your recovery at each stage.
Immediate Post-Operative Period (Days 0-3)
Hospital Stay (1-3 Days)
Day of Surgery:
- Recovery in PACU (Post-Anesthesia Care Unit)
- Pain management initiated
- Ice therapy applied to knee
- Compression device to prevent blood clots
- Physical therapy may begin same day in some protocols
Goals:
- Pain control
- Prevention of complications
- Early mobilization
- Basic self-care education
Exercises Begin Immediately:
Ankle Pumps:
- Move ankle up and down
- 10 repetitions every hour while awake
- Prevents blood clots and reduces swelling
Quadriceps Sets:
- Tighten thigh muscle, push knee down into bed
- Hold 5 seconds, repeat 10 times
- Perform every 2-3 hours
Gluteal Sets:
- Squeeze buttock muscles together
- Hold 5 seconds, repeat 10 times
- Every 2-3 hours
Early Mobilization:
- Sit up in chair within 6-12 hours
- Stand and take first steps with physical therapist
- Use walker or crutches for support
- Practice getting in and out of bed safely
Pain Management
Multimodal Approach:
- Nerve blocks (may last 12-24 hours)
- Oral pain medications (opioids and non-opioids)
- Anti-inflammatory medications
- Ice therapy (20 minutes every 2-3 hours)
- Elevation above heart level
Pain Expectations:
- Moderate to severe pain first 2-3 days
- Pain should gradually decrease each day
- Take medications as prescribed, not just when severe
Wound Care
- Dressing typically stays on 3-7 days
- Keep surgical site clean and dry
- No soaking in bath or pool initially
- Watch for signs of infection (increased redness, warmth, drainage, fever)
Prevention of Complications
Deep Vein Thrombosis (DVT) Prevention:
- Blood thinning medication
- Compression stockings
- Sequential compression devices
- Early mobilization
- Ankle pumps and leg exercises
Infection Prevention:
- Proper wound care
- Antibiotics as prescribed
- Hand hygiene
- Monitor for fever or increasing pain
Early Recovery Phase (Weeks 1-2)
Home Setup Before Surgery
Bedroom:
- Firm chair with armrests
- Elevated toilet seat
- Reacher/grabber tool
- Long-handled shoe horn
- Sock aid device
Safety:
- Remove throw rugs
- Install handrails on stairs
- Clear walking paths
- Non-slip mats in bathroom
- Good lighting throughout home
Daily Exercise Program
Frequency: 3-4 times daily, 20-30 minutes per session
Essential Exercises:
- Heel Slides (Knee Flexion):
- Lie on back
- Slide heel toward buttocks, bending knee
- Hold 5 seconds
- 10 repetitions, 3 sets
- Straight Leg Raises:
- Tighten quadriceps
- Lift leg 6-12 inches off bed
- Hold 5 seconds, lower slowly
- 10 repetitions, 3 sets
- Progress to standing as strength improves
- Short Arc Quads:
- Place rolled towel under knee
- Straighten knee, lifting foot
- Hold 5 seconds
- 10 repetitions, 3 sets
- Knee Extension:
- Sit in chair, place foot on stool
- Place rolled towel under ankle
- Push knee down toward floor
- Hold 10-30 seconds
- Repeat 5-10 times
- Ankle Pumps:
- Continue throughout recovery
- Every hour while awake
Walking:
- Walk short distances multiple times daily
- Use walker initially, progress to cane
- Gradually increase distance each day
- Week 1: Walk 50-100 feet, 4-6 times daily
- Week 2: Walk 100-300 feet, 4-6 times daily
Range of Motion Goals
Week 1:
- Extension: 0 degrees (straight leg)
- Flexion: 60-70 degrees
Week 2:
- Extension: 0 degrees
- Flexion: 80-90 degrees
Activity Guidelines
DO:
- Ice knee 20 minutes after exercises
- Elevate leg when sitting
- Sleep on back or non-surgical side
- Use assistive devices as recommended
- Take pain medication before exercises
DON’T:
- Twist or pivot on surgical leg
- Cross legs
- Kneel on surgical knee
- Lift more than 10 pounds
- Drive until cleared by surgeon (typically 4-6 weeks)
Intermediate Phase (Weeks 3-6)
Physical Therapy
Outpatient PT typically begins:
- 2-3 times per week
- Progress exercises under supervision
- Manual therapy for scar mobilization
- Modalities (heat, ice, electrical stimulation)
- Gait training
Advanced Exercises
- Mini Squats:
- Stand holding counter for support
- Bend knees 30-45 degrees
- Hold 5 seconds
- 10 repetitions, 3 sets
- Step-Ups:
- Start with 4-inch step, progress to 8 inches
- Step up with surgical leg
- 10 repetitions each leg
- 2-3 sets
- Seated Knee Extension with Resistance:
- Use ankle weights or resistance band
- Start with 1-2 pounds
- 10-15 repetitions, 3 sets
- Hamstring Curls (Standing):
- Hold counter for support
- Bend knee, bringing heel toward buttock
- 10-15 repetitions, 3 sets
- Add ankle weights as tolerated
- Hip Abduction:
- Stand with support
- Lift leg out to side
- Keep toes pointing forward
- 10-15 repetitions, 3 sets
- Stationary Bike:
- Begin when can achieve 90-100 degrees flexion
- Start with 5-10 minutes
- No resistance initially
- Gradually increase time and resistance
Range of Motion Goals
Week 3-4:
- Flexion: 90-100 degrees
Week 5-6:
- Flexion: 100-110 degrees
- Extension: 0 degrees (full)
Functional Activities
By Week 6:
- Walking without assistive device (most patients)
- Light household chores
- Short car rides as passenger
- May drive if approved by surgeon
- Return to desk work possible
- Sleeping in any position comfortable
Recovery Phase (Weeks 7-12)
Strengthening Focus
Intensity Increases:
- Add resistance to all exercises
- Longer duration cardio activities
- More functional movements
Advanced Exercises:
- Wall Slides:
- Back against wall
- Slide down to 45-60 degree bend
- Hold 10 seconds
- 10 repetitions
- Lateral Step-Ups:
- Step sideways onto platform
- Return to start
- 10 repetitions each side
- Partial Lunges:
- Step forward, bend both knees
- Keep front knee over ankle
- 10 repetitions each leg
- Calf Raises:
- Rise up on toes
- Hold 5 seconds
- 15-20 repetitions
- Leg Press Machine:
- Begin with light weight
- Gradually increase resistance
- 2-15 repetitions, 3 sets
Cardiovascular Exercise
- Walking 30-45 minutes daily
- Stationary bike 20-30 minutes
- Swimming or water aerobics (when incision healed)
- Elliptical machine (low impact)
Range of Motion Goals
Week 12:
- Flexion: 115-120 degrees (goal)
- Extension: 0 degrees
Functional Milestones
By 12 Weeks:
- Independent with all daily activities
- Walking unlimited distances
- Driving regularly
- Light recreational activities
- Return to most work activities
- Stairs without difficulty
Long-Term Recovery (Months 4-12)
Months 4-6
Exercise Progression:
- Continue strengthening program
- Add variety to prevent plateaus
- Consider gym membership or home equipment
- Focus on balance and proprioception
Activities:
- Return to golf (most patients)
- Swimming, cycling unlimited
- Light hiking
- Doubles tennis (check with surgeon)
- Dancing
Months 7-12
Final Strengthening:
- Near-normal strength in surgical leg
- Minimal to no swelling
- Full range of daily activities without limitation
Return to Sports:
- Low-impact sports encouraged
- High-impact sports generally discouraged
- Individual assessment by surgeon
Recommended:
- Walking, hiking
- Swimming, water aerobics
- Cycling, stationary bike
- Golf
- Doubles tennis
- Ballroom dancing
- Tai chi, yoga (modified)
Not Recommended:
- Running, jogging
- Singles tennis
- Basketball
- Soccer
- Skiing (discuss with surgeon)
- Contact sports
Red Flags – When to Contact Surgeon
Call Immediately If:
- Fever over 101°F (38.3°C)
- Increasing redness, warmth, or drainage from incision
- Sudden increase in pain not relieved by medication
- Calf pain, swelling, or warmth (possible blood clot)
- Shortness of breath or chest pain
- Inability to bear weight
- Feeling of knee giving way
Tips for Optimal Recovery
Nutrition
- High protein diet for healing (0.8-1.0 g/kg body weight)
- Adequate calcium and vitamin D
- Stay well hydrated
- Iron-rich foods if anemic
- Consider protein supplements if needed
Sleep
- Use pillows for positioning comfort
- Ice before bed to reduce pain
- Take pain medication as needed
- Sleep is critical for healing
Mental Health
- Set realistic expectations
- Recovery is not linear – expect ups and downs
- Stay connected with support system
- Consider counseling if feeling depressed
- Join support groups (online or in-person)
Weight Management
- Maintain healthy weight to reduce stress on implant
- Extra weight increases wear on components
- Combine diet with increased activity
Expected Timeline Summary
Week 1-2: Focus on pain management, wound healing, basic mobility
Week 3-6: Progress range of motion, begin outpatient PT, increase strength
Week 7-12: Continue strengthening, return to most daily activities
Month 4-6: Near-normal function, return to recreational activities
Month 7-12: Maximize strength and function, unrestricted low-impact activities
Year 1+: Long-term maintenance, protect implant longevity
Long-Term Implant Care
- Continue regular exercise to maintain muscle strength
- Avoid excessive weight gain
- Inform dentist about knee replacement (antibiotic prophylaxis)
- Regular follow-up with orthopedic surgeon (yearly after initial recovery)
- Report any new pain or concerns promptly
- Expect implant to last 15-20+ years with proper care
Conclusion
Recovery from total knee replacement requires patience, dedication, and consistent effort. While the timeline provided is typical, remember that everyone heals at their own pace. Stay in close communication with your surgical team, follow your prescribed exercise program diligently, and don’t hesitate to ask questions. The majority of patients experience excellent pain relief and significant functional improvement, making the recovery process worthwhile. Your commitment to rehabilitation is the key to achieving the best possible outcome.