Introduction
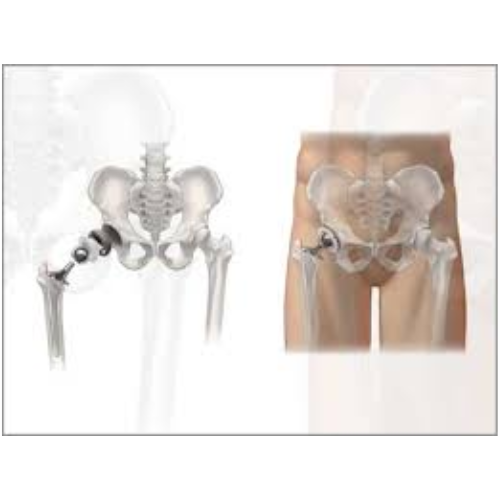
Total hip replacement (THR) is one of the most successful orthopedic procedures, offering dramatic pain relief and improved function. However, achieving optimal outcomes requires adherence to a structured recovery protocol. This comprehensive guide will help you navigate each phase of your recovery journey.
Understanding Hip Precautions
The specific precautions depend on your surgical approach. Always follow your surgeon’s specific instructions.
Posterior Approach Precautions (Most Common)
Avoid for 6-12 Weeks:
– No Hip Flexion Beyond 90 Degrees: Don’t bend hip past right angle
– No Hip Adduction: Don’t cross legs or bring operated leg past midline
– No Internal Rotation: Don’t turn toes inward or twist toward midline
The “3 Big No’s”:
1. Don’t bend too far forward
2. Don’t cross your legs
3. Don’t pivot or twist on the surgical leg
Anterior Approach Precautions (Less Restrictive)
Avoid for 6-12 Weeks:
– No Hip Extension: Avoid bringing leg behind body
– No External Rotation: Don’t turn toes outward excessively
– No Hyperextension: Don’t overextend the hip backward
Generally allows:
– Earlier return to normal activities
– Fewer movement restrictions
– May cross legs sooner (check with surgeon)
Lateral Approach Precautions
Avoid:
– No Hip Adduction: Don’t cross legs past midline
– No Combined Movements: Avoid twisting while bending
Immediate Post-Operative Period (Days 0-2)
Hospital Stay (1-2 Days)
Day of Surgery:
– Recovery room monitoring
– Pain management initiated
– Abductor pillow or wedge between legs
– Compression stockings applied
– Physical therapy evaluation
First Evening/Next Morning:
– Sit up in chair with assistance
– Stand with walker
– May take first steps
– Begin exercise program
Early Exercises (Begin Day of Surgery)
Ankle Pumps:
– Point toes up and down
– Circle ankles both directions
– 10-20 repetitions every hour awake
– Prevents blood clots
Quadriceps Sets:
– Tighten thigh muscles
– Push back of knee down
– Hold 5 seconds, repeat 10 times
– Every 2-3 hours
Gluteal Squeezes:
– Tighten buttock muscles
– Hold 5 seconds, repeat 10 times
– Strengthens hip muscles
Heel Slides (if approved for your approach):
– Slide heel up, bending knee
– Keep hip restrictions in mind
– 10 repetitions, 3-4 times daily
Pain Management
Medications:
– Multimodal approach (opioids, NSAIDs, acetaminophen)
– Nerve blocks may provide 12-24 hours relief
– Regular dosing schedule initially
– Transition to as-needed basis
Non-Pharmacological:
– Ice packs 20 minutes, 4-6 times daily
– Elevation when sitting
– Proper positioning
– Relaxation techniques
Early Mobility
Day 1-2 Goals:
– Sit in chair 2-3 times daily
– Walk 50-100 feet with walker
– Transfer safely (bed, chair, toilet)
– Understand hip precautions thoroughly
DVT Prevention
Critical First Week:
– Blood thinning medication (2-6 weeks typically)
– Compression stockings
– Sequential compression devices
– Early mobilization
– Ankle exercises every hour
– Adequate hydration
Week 1-2: Early Home Recovery
Home Preparation Essentials
Bedroom/Bathroom:
– Elevated toilet seat (2-4 inches)
– Shower chair or bench
– Handheld showerhead
– Grab bars in shower/tub
– Remove rugs and tripping hazards
Daily Living Aids:
– Reacher/grabber (24-32 inches)
– Long-handled shoe horn
– Sock aid device
– Dressing stick
– Long-handled sponge
Furniture:
– Firm chair with armrests (seat height 18-20 inches)
– No low sofas or recliners
– Recliner chair is acceptable if can maintain precautions
Daily Exercise Program
Frequency: 3-4 times per day, 15-20 minutes each session
Essential Exercises:
- Ankle Pumps (Continue from hospital)
– Every hour while awake
– 10-20 repetitions - Quadriceps Sets
– Tighten thigh, hold 5 seconds
– 10 repetitions, 3 sets
– Perform on both legs - Gluteal Sets
– Squeeze buttocks together
– Hold 5 seconds
– 10 repetitions, 3 sets - Hip Abduction (Lying)
– Lie on back
– Slide leg out to side 12 inches
– Keep toes pointing up
– 10 repetitions, 3 sets - Hip Extension (Standing)
– Hold counter for balance
– Lift leg backward (only if anterior approach)
– Don’t arch back
– 10 repetitions, 3 sets - Short Arc Quads
– Roll towel under knee
– Straighten knee, lifting foot
– Hold 5 seconds
– 10 repetitions, 3 sets
Walking Program
Week 1:
– Walk 100-200 feet, 4-6 times daily
– Use walker for all walking
– Take small steps
– Even weight on both legs
Week 2:
– Walk 200-400 feet, 4-6 times daily
– May progress to crutches if approved
– Increase distance gradually
Activities of Daily Living
Sitting:
– Use elevated toilet seat
– Choose chairs with armrests
– Don’t sit on low surfaces
– Keep hips higher than knees
– Don’t lean forward excessively
Dressing:
– Dress operated leg first
– Use long-handled devices
– Put pants/underwear on while lying down
– Slip-on shoes initially
Bathing:
– Sponge bath first few days
– Shower when wound sealed (usually 5-7 days)
– Use shower chair
– Don’t bend to wash feet – use long-handled sponge
Sleeping:
– Sleep on back with pillow between legs
– May sleep on non-operative side with pillow between legs
– Don’t sleep on operative side for 6 weeks
– Keep pillow between legs while sleeping
What to Avoid
DO NOT:
– Bend hip beyond 90 degrees (posterior approach)
– Cross legs or ankles
– Twist or pivot on operated leg
– Sit on low surfaces
– Reach to tie shoes (use aids)
– Drive (typically 4-6 weeks)
– Have sexual activity (discuss with surgeon, typically 4-6 weeks)
Weeks 3-6: Building Strength and Independence
Physical Therapy Begins
Outpatient PT (2-3 times weekly):
– Gait training and balance
– Progressive strengthening
– Range of motion work
– Scar mobilization
– Manual therapy
Progressive Exercises
- Standing Hip Abduction
– Hold counter for support
– Lift leg out to side
– Keep toes forward
– 10-15 repetitions, 3 sets - Standing Hip Extension
– Lift leg backward
– Don’t arch back
– 10-15 repetitions, 3 sets - Mini Squats
– Feet shoulder-width apart
– Hold counter, bend knees 30 degrees
– Keep back straight
– 10 repetitions, 3 sets - Step-Ups
– Start with 4-inch step
– Step up with operated leg
– 10 repetitions, 2-3 sets - Stationary Bike
– Begin when flexibility allows
– Seat high enough to avoid flexion >90°
– Start 5-10 minutes, no resistance
– Progress to 20-30 minutes - Bridging
– Lie on back, knees bent
– Lift buttocks off bed
– Hold 5 seconds
– 10-15 repetitions, 2-3 sets - Clamshells
– Lie on non-operative side
– Knees bent, feet together
– Lift top knee
– 10-15 repetitions, 3 sets
Walking Progression
Week 3-4:
– Walk 500-1000 feet, multiple times daily
– Progress to one crutch or cane if approved
– Use cane in opposite hand from surgery
Week 5-6:
– Walk 15-30 minutes continuously
– May walk without assistive device if gait normal
– Add outdoor walking on even surfaces
Functional Milestones
By Week 6:
– Independent with self-care
– Walking with minimal or no assistive device
– Light household activities
– May drive if approved and off narcotics
– Return to desk work possible
Weeks 7-12: Advancing Function
Exercise Progression
Increase Intensity:
– Add ankle weights (1-2 pounds, progress to 5 pounds)
– Increase repetitions to 15-20
– Add resistance bands
– Longer duration cardio
Advanced Exercises:
- Wall Squats
– Back against wall
– Slide down to 45 degrees
– Hold 10 seconds
– 10 repetitions - Lateral Step-Ups
– Step sideways onto platform
– 6-8 inch height
– 10 repetitions each direction - Partial Lunges
– When cleared by therapist
– Keep front knee over ankle
– Small range initially - Single Leg Stance
– Balance on operated leg
– Hold counter if needed
– Progress to no support
– Hold 30 seconds, repeat 5 times - Heel Raises
– Rise up on toes
– Hold 3 seconds
– 15-20 repetitions
Cardiovascular Exercise
– Walking 30-45 minutes daily
– Stationary bike 20-30 minutes
– Swimming (when incision fully healed, typically 6 weeks)
– Water aerobics (excellent low-impact option)
Discontinuing Hip Precautions
Typically at 6-12 Weeks (varies by surgeon):
– May cross legs
– May bend beyond 90 degrees
– May reach to tie shoes
– May resume normal sitting postures
– Continue to avoid extreme positions
Activity Progression
Weeks 8-12:
– Return to most work activities
– Light gardening
– Golf (check with surgeon)
– Dancing
– Sexual activity (discuss with surgeon)
– Travel short distances
Months 4-6: Returning to Life
Final Strengthening Phase
Goals:
– Restore muscle strength to 80-90% of non-operative leg
– Eliminate compensation patterns
– Maximize functional independence
Exercise Program:
– Continue strengthening 3-4 times weekly
– Add variety to prevent boredom
– Consider gym membership
– Group fitness classes (modified as needed)
Return to Recreation
Low-Impact Activities (Recommended):
– Swimming and water aerobics
– Cycling (road and stationary)
– Walking and hiking
– Golf
– Doubles tennis
– Dancing (ballroom, social)
– Yoga (modified, avoid extreme positions)
– Tai chi
– Elliptical machine
Moderate-Impact (Discuss with Surgeon):
– Singles tennis
– Light jogging (controversial, many surgeons discourage)
– Cross-country skiing
– Low-impact aerobics
High-Impact (Generally Not Recommended):
– Running
– Basketball
– Soccer
– Racquetball
– High-impact aerobics
– Gymnastics
– Contact sports
Functional Expectations
By 6 Months:
– Near-normal walking
– Able to perform all daily activities
– Return to most recreational activities
– Minimal to no pain
– Occasional mild aching normal
– Slight leg length difference may be noticeable
Long-Term Care (6 Months – Lifelong)
Ongoing Exercise
Maintain Strength:
– Continue exercise program 3-4 times weekly
– Focus on hip abductors and extensors
– Core strengthening
– Balance exercises
Lifetime Activity:
– Regular low-impact exercise
– Maintain healthy weight
– Stay active for implant longevity
Activity Modifications
Protect Your Hip:
– Avoid repetitive high-impact activities
– Use good body mechanics
– Don’t ignore pain signals
– Modify activities as needed
Infection Prevention
Dental Work:
– Inform dentist about hip replacement
– May need antibiotics before procedures (first 2 years typically)
Other Procedures:
– Tell all healthcare providers about hip replacement
– May need antibiotics before invasive procedures
Regular Follow-Up
Surgeon Visits:
– 6 weeks, 3 months, 6 months, 1 year
– Then annually
– X-rays to monitor implant
Report Changes:
– New or increasing pain
– Changes in mobility
– Grinding or clicking sensations
– Any concerns about hip
Warning Signs – Contact Surgeon
Call Immediately:
– Fever over 101°F (38.3°C)
– Increasing wound redness, warmth, drainage
– Severe pain not controlled by medication
– Leg swelling, warmth, redness (blood clot)
– Chest pain or shortness of breath
– Hip feels like it “pops out”
– Sudden inability to bear weight
Call Soon:
– Persistent groin or thigh pain
– New clicking or grinding
– Increased swelling
– Feeling unstable or insecure
Tips for Success
Nutrition
– High protein for healing (75-100g daily)
– Calcium and vitamin D for bone health
– Iron if anemic
– Stay well hydrated
– Maintain healthy weight
Sleep
– Use pillow between legs
– May take time to find comfortable position
– Ice before bed
– Proper pain management
Mental Health
– Recovery takes time – be patient
– Some days better than others
– Stay connected with support system
– Consider counseling if needed
– Join hip replacement support groups
Realistic Expectations
– Full recovery takes 6-12 months
– Improvement continues up to 2 years
– 95% of patients very satisfied
– Most experience dramatic pain relief
– Return to active lifestyle expected
Conclusion
Recovery from hip replacement requires commitment and patience, but the results are typically excellent. Most patients experience dramatic pain relief and return to an active lifestyle. Follow your surgeon’s specific instructions, attend all therapy appointments, and progress at your own pace. Remember that everyone heals differently – comparing yourself to others isn’t helpful. Stay focused on your own progress, communicate with your healthcare team, and trust the process. The effort you invest in rehabilitation will pay dividends in your quality of life for years to come.