Introduction
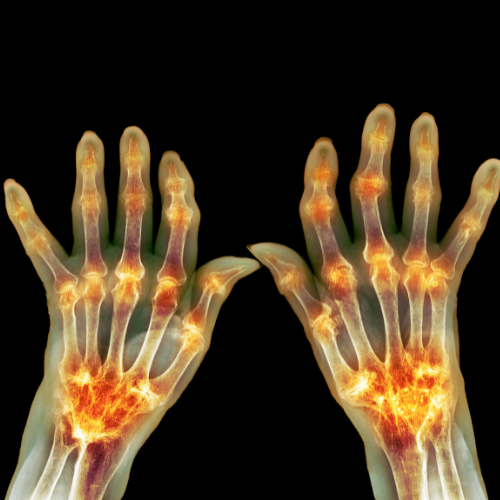
Inflammatory arthritis refers to a group of conditions characterized by inflammation of the joints caused by an overactive immune system. Unlike osteoarthritis, which results from wear and tear, inflammatory arthritis involves autoimmune or autoinflammatory processes attacking the joints. This comprehensive guide will help you understand these conditions, their impact on musculoskeletal health, and management strategies from an orthopedic perspective.
Understanding Inflammatory Arthritis
What is Inflammatory Arthritis?
Inflammatory arthritis encompasses various conditions where the immune system mistakenly attacks the synovium (joint lining), leading to:
– Persistent joint inflammation
– Synovial thickening and excess fluid production
– Progressive cartilage and bone damage
– Potential systemic involvement beyond joints
Key Differences from Osteoarthritis
Inflammatory Arthritis:
– Autoimmune or autoinflammatory process
– Affects multiple joints symmetrically (often)
– Morning stiffness >30-60 minutes
– Systemic symptoms (fatigue, fever)
– Elevated inflammatory markers (ESR, CRP)
– Can affect young people
– Requires disease-modifying medications
Osteoarthritis:
– Degenerative, mechanical wear
– Asymmetric joint involvement
– Morning stiffness <30 minutes
– No systemic symptoms
– Normal inflammatory markers
– Primarily affects older adults
– Treated with pain management and physical therapy
Types of Inflammatory Arthritis
1. Rheumatoid Arthritis (RA)
Most Common Inflammatory Arthritis
Characteristics:
– Autoimmune condition
– Symmetrical polyarthritis (multiple joints)
– Small joints of hands and feet primarily affected
– Affects 1% of population
– Women 3x more common than men
– Peak onset 30-60 years
Joint Involvement:
– Metacarpophalangeal (MCP) joints
– Proximal interphalangeal (PIP) joints
– Wrists
– Metatarsophalangeal (MTP) joints
– Knees, ankles, shoulders, elbows (later stages)
– Cervical spine (particularly C1-C2, dangerous)
Characteristic Features:
– Rheumatoid nodules (20-30% of patients)
– Swan-neck and boutonniere deformities (hands)
– Ulnar deviation of fingers
– Carpal tunnel syndrome common
– Atlantoaxial instability (spine)
Diagnostic Criteria:
– Morning stiffness >1 hour
– Arthritis of 3+ joint areas
– Arthritis of hand joints
– Symmetrical arthritis
– Rheumatoid nodules
– Positive rheumatoid factor (RF) or anti-CCP antibodies
– Elevated ESR or CRP
Orthopedic Complications:
– Progressive joint destruction
– Tendon ruptures (especially extensor tendons of hand)
– Carpal tunnel syndrome
– Cervical instability (requires pre-operative evaluation)
– Joint deformities requiring reconstruction
2. Psoriatic Arthritis (PsA)
Arthritis Associated with Psoriasis
Characteristics:
– Inflammatory arthritis in patients with psoriasis
– 30% of psoriasis patients develop arthritis
– Can precede skin disease (10-15% of cases)
– Equal gender distribution
– Peak onset 30-50 years
Joint Involvement Patterns:
– Asymmetric oligoarthritis (most common): Few joints, asymmetric
– Symmetric polyarthritis: Similar to RA
– DIP predominant: Distal finger joints
– Spondylitis: Spine and sacroiliac joints
– Arthritis mutilans: Severe destructive (rare)
Characteristic Features:
– Dactylitis (“sausage digits”): entire finger/toe swelling
– Enthesitis: inflammation at tendon insertions
– Nail changes (pitting, onycholysis)
– Psoriatic skin plaques
– Asymmetric pattern often
Diagnostic Features:
– Psoriasis (current or history)
– Dactylitis
– Nail changes
– Negative rheumatoid factor (seronegative)
– Radiographic findings (pencil-in-cup deformity)
Orthopedic Implications:
– Axial involvement (spine, SI joints)
– Enthesitis (Achilles, plantar fascia)
– Joint destruction can be severe
– May require joint replacement
3. Ankylosing Spondylitis (AS)
Inflammatory Arthritis of the Spine
Characteristics:
– Primarily affects axial skeleton
– Chronic inflammatory disease
– HLA-B27 associated (90% of patients)
– Men 3x more common than women
– Onset typically 15-35 years
Primary Involvement:
– Sacroiliac joints (early and hallmark)
– Spine (ascending pattern)
– Hip and shoulder joints (30-40%)
– Peripheral joints less common
– Enthesitis common
Characteristic Features:
– Inflammatory back pain (worse at night, better with movement)
– Morning stiffness >30 minutes
– Loss of spinal mobility
– Reduced chest expansion
– Bamboo spine (late stage)
– Stooped posture
Diagnostic Criteria (ASAS Criteria):
– Sacroiliitis on imaging PLUS
– Back pain >3 months, onset <45 years
– Or HLA-B27 positive with 2+ SpA features
Orthopedic Complications:
– Progressive spinal fusion
– Spinal fractures (rigid spine vulnerable)
– Hip involvement requiring replacement
– Thoracic restriction affecting breathing
– Cervical spine involvement
4. Reactive Arthritis (Formerly Reiter’s Syndrome)
Post-Infectious Arthritis
Characteristics:
– Develops after infection (GI or GU)
– HLA-B27 associated (60-80%)
– More common in men
– Usually self-limited
Triggering Infections:
– Chlamydia (genitourinary)
– Salmonella, Shigella, Campylobacter (GI)
– Yersinia
Classic Triad:
– Arthritis (primarily lower extremity)
– Urethritis
– Conjunctivitis
Joint Involvement:
– Asymmetric oligoarthritis
– Knees, ankles, feet most common
– Sacroiliitis can occur
– Enthesitis common (Achilles, plantar fascia)
Orthopedic Features:
– Usually self-limited (months)
– 15-50% develop chronic arthritis
– Dactylitis possible
– Heel pain from enthesitis
5. Gout and Pseudogout (Crystal Arthropathies)
Inflammatory Arthritis from Crystal Deposition
Gout
Characteristics:
– Monosodium urate crystal deposition
– Hyperuricemia (elevated uric acid)
– Men 4x more common than women
– Peak onset 40-50 years
Classic Presentation:
– Acute, severe monoarthritis
– First metatarsophalangeal joint (big toe, “podagra”) most common
– Sudden onset, often overnight
– Exquisitely painful
– Red, hot, swollen joint
Chronic Gout:
– Tophaceous deposits (tophi)
– Polyarticular involvement
– Joint destruction
– Kidney stones
Orthopedic Implications:
– Severe erosions
– Tophi causing masses, nerve compression
– May require surgical debulking
– Joint destruction requiring replacement
Pseudogout (CPPD – Calcium Pyrophosphate Deposition)
Characteristics:
– Calcium pyrophosphate crystal deposition
– Older adults (>60 years typically)
– Equal gender distribution
Joint Involvement:
– Knees most common
– Wrists
– Shoulders
– Often mimics other arthritis types
Orthopedic Considerations:
– May resemble infection or gout
– Can accelerate osteoarthritis
– Associated with chondrocalcinosis on X-ray
6. Juvenile Idiopathic Arthritis (JIA)
Inflammatory Arthritis in Children
Characteristics:
– Onset before age 16
– Multiple subtypes
– Can cause growth disturbances
– Requires specialized pediatric rheumatology care
Orthopedic Implications:
– Limb length discrepancies
– Joint contractures
– Growth plate involvement
– TMJ involvement common
– May require early joint replacement
7. Enteropathic Arthritis
Associated with Inflammatory Bowel Disease
Characteristics:
– Occurs in Crohn’s disease or ulcerative colitis
– 10-20% of IBD patients develop arthritis
– Peripheral or axial arthritis
Types:
– Type 1: Pauciarticular, asymmetric, large joints
– Type 2: Polyarticular, symmetric, small joints
– Axial: Similar to ankylosing spondylitis
Orthopedic Features:
– Often parallels bowel disease activity
– Usually non-erosive
– Good response to IBD treatment
General Signs and Symptoms
Joint Symptoms
Pain:
– Worse with rest, improves with movement
– Night pain common
– Present even at rest
Stiffness:
– Morning stiffness >30-60 minutes (hallmark)
– Gelling phenomenon (stiffness after inactivity)
– Improves with movement
Swelling:
– Soft tissue swelling
– Joint effusions
– Warm to touch
– Boggy, synovial thickening
Loss of Function:
– Reduced range of motion
– Difficulty with fine motor tasks
– Grip weakness
– Trouble with stairs, walking
Systemic Symptoms
Constitutional:
– Fatigue (very common)
– Low-grade fever
– Weight loss
– Malaise
Extra-Articular Manifestations:
– Eye inflammation (uveitis, scleritis)
– Skin changes (nodules, rashes)
– Lung involvement
– Cardiovascular complications
– Kidney involvement
– Neurological symptoms
Diagnosis
Clinical Evaluation
History:
– Pattern of joint involvement
– Duration and progression
– Morning stiffness duration
– Systemic symptoms
– Family history
– Previous infections
– Skin or eye problems
Physical Examination:
– Joint examination (swelling, tenderness, warmth)
– Range of motion assessment
– Deformity evaluation
– Spine examination
– Skin examination
– Eye examination
– Systemic examination
Laboratory Tests
Inflammatory Markers:
– ESR (erythrocyte sedimentation rate): elevated
– CRP (C-reactive protein): elevated
– Monitor disease activity
Autoantibodies:
– Rheumatoid factor (RF): RA
– Anti-CCP antibodies: RA (more specific)
– ANA (antinuclear antibody): Various conditions
– HLA-B27: Ankylosing spondylitis, reactive arthritis
Other Tests:
– Complete blood count (anemia common)
– Liver and kidney function
– Uric acid (gout)
– Joint fluid analysis (if effusion present)
Joint Fluid Analysis:
– Cell count (inflammatory >2000 WBC)
– Crystal analysis (gout, pseudogout)
– Culture (rule out infection)
– Gram stain
Imaging Studies
X-rays
Early Changes:
– Soft tissue swelling
– Periarticular osteopenia
– Joint space narrowing (later)
Late Changes:
– Erosions (hallmark of RA)
– Joint destruction
– Subluxations and deformities
– Ankylosis (fusion)
– Specific patterns (e.g., pencil-in-cup in PsA)
MRI
Advantages:
– Detects early synovitis
– Shows bone marrow edema
– Identifies erosions before visible on X-ray
– Assesses soft tissue involvement
– Useful for spine (AS)
Ultrasound
Benefits:
– Detects synovitis and effusions
– Power Doppler shows active inflammation
– Guides injections
– Point-of-care assessment
– No radiation
CT Scan
Uses:
– Bone detail (erosions)
– Sacroiliac joints (AS)
– Surgical planning
Treatment Approach
Goals of Treatment
1. Control inflammation and prevent damage
2. Relieve pain and improve function
3. Prevent or minimize joint destruction
4. Maintain quality of life
5. Minimize treatment side effects
Multidisciplinary Care Team
– Rheumatologist (primary medical management)
– Orthopedic surgeon (surgical interventions)
– Physical therapist
– Occupational therapist
– Pain specialist
– Podiatrist (foot involvement)
– Ophthalmologist (eye involvement)
– Primary care physician
Medical Treatment (Rheumatology)
Disease-Modifying Anti-Rheumatic Drugs (DMARDs)
Conventional DMARDs
Methotrexate (Gold Standard for RA):
– First-line therapy
– Weekly dosing
– Requires folic acid supplementation
– Monitor liver and blood counts
Sulfasalazine:
– Used in RA, SpA, PsA
– GI side effects common
Hydroxychloroquine:
– Mild disease or combination therapy
– Eye monitoring required
Leflunomide:
– Alternative to methotrexate
– Similar efficacy
Biologic DMARDs
TNF Inhibitors:
– Etanercept, adalimumab, infliximab, golimumab, certolizumab
– Highly effective for RA, PsA, AS
– Subcutaneous or IV administration
– Risk of infections, reactivation TB
Non-TNF Biologics:
– Rituximab (anti-CD20)
– Abatacept (T-cell inhibitor)
– Tocilizumab (IL-6 inhibitor)
– Anakinra (IL-1 inhibitor)
IL-17 and IL-23 Inhibitors:
– Secukinumab, ixekizumab (IL-17)
– Ustekinumab, guselkumab (IL-23)
– Particularly effective for PsA and AS
JAK Inhibitors (Targeted Synthetic DMARDs)
Examples:
– Tofacitinib, baricitinib, upadacitinib
– Oral medication (advantage over biologics)
– Effective for RA, PsA
– Monitor for infections, clots
NSAIDs and Analgesics
NSAIDs:
– Reduce pain and inflammation
– Not disease-modifying
– First-line for AS symptoms
– GI and cardiovascular precautions
Analgesics:
– Acetaminophen for pain
– Opioids rarely indicated
– Topical agents
Corticosteroids
Systemic:
– Bridging therapy while DMARDs take effect
– Lowest effective dose
– Short-term use preferred
– Taper as able
Intra-Articular Injections:
– Target specific symptomatic joints
– Provide temporary relief (weeks to months)
– Limit frequency (3-4 per year per joint)
– Useful as bridge or for flares
Orthopedic Treatment and Surgery
Non-Surgical Orthopedic Management
Orthotics and Splints:
– Wrist splints for RA
– Ankle-foot orthoses
– Custom foot orthoses
– Cervical collar (cervical involvement)
Assistive Devices:
– Canes, walkers
– Jar openers, button hooks
– Built-up utensil handles
– Elevated toilet seats
– Shoe modifications
Bracing:
– Knee braces for stability
– Ankle braces
– Thumb splints
Indications for Orthopedic Surgery
Pain:
– Severe, persistent pain despite medical management
– Pain interfering with sleep and function
– Failed conservative and medical treatment
Function:
– Significant functional limitation
– Unable to perform activities of daily living
– Inability to work or enjoy life
Deformity:
– Progressive deformity
– Instability
– Tendon ruptures
Joint Destruction:
– Severe radiographic damage
– Bone-on-bone arthritis
– Failed joints
Common Orthopedic Procedures
Joint Replacement (Arthroplasty)
Most Common:
– Total hip replacement
– Total knee replacement
– Shoulder replacement
– Total ankle replacement
– Small joint replacements (fingers, wrist)
Considerations in Inflammatory Arthritis:
– Younger age at surgery (compared to OA)
– Multiple joint involvement
– May need staged procedures
– Higher revision rates in some conditions
– Bone quality concerns (osteoporosis)
– Need to coordinate with rheumatologist
– Infection risk with immunosuppression
Timing:
– Control disease activity before surgery
– Discontinue some medications perioperatively
– Coordinate with rheumatology
Synovectomy
Procedure:
– Removal of inflamed synovium
– Arthroscopic or open
– Delays joint destruction
Indications:
– Persistent synovitis despite medical management
– Before significant joint damage
– Most effective when done early
Common Sites:
– Wrist
– Knee
– Elbow
– Ankle
Outcomes:
– Temporary relief (synovium can regrow)
– Delays but doesn’t prevent damage
– Best results in early disease
Tendon Surgery
Tendon Rupture Repair:
– Common in RA (extensor tendons of hand)
– Requires prompt surgical repair
– Tendon transfers may be needed
Tendon Synovectomy:
– Remove inflamed tenosynovium
– Prevent tendon rupture
– Commonly in hand/wrist
Arthrodesis (Fusion)
Indications:
– Severe joint destruction
– When replacement not ideal
– Instability
Common Sites:
– Wrist
– Ankle
– Thumb (CMC joint)
– Toes (MTP joints)
– Cervical spine (instability)
Advantages:
– Pain relief
– Stability
– Durability
Disadvantages:
– Loss of motion
– Adjacent joint stress
Reconstructive Hand Surgery
Common Procedures:
– MCP joint replacement or fusion
– Wrist arthrodesis or arthroplasty
– Tendon transfers
– Boutonniere or swan-neck correction
Goals:
– Restore function
– Correct deformity
– Relieve pain
– Improve appearance
Spine Surgery
Indications:
– Atlantoaxial instability (RA)
– Neurological compromise
– Severe deformity (AS)
– Spinal fractures
Procedures:
– Cervical fusion (C1-C2)
– Decompression
– Corrective osteotomy (AS)
Considerations:
– High-risk procedures
– Requires experienced surgeon
– Pre-operative imaging essential
Pre-Operative Considerations
Medical Optimization:
– Achieve remission or low disease activity if possible
– Optimize nutrition (anemia common)
– Smoking cessation
– Dental clearance
– Control comorbidities
Medication Management:
– Coordinate with rheumatologist
– Timing of DMARD discontinuation varies:
* Methotrexate: Usually continue
* TNF inhibitors: Hold 1-2 weeks before, resume when healing
* Rituximab: Difficult timing
* Corticosteroids: Continue, possible stress dose
– Individual protocols vary by surgeon and medication
Infection Risk:
– Higher with immunosuppression
– Prophylactic antibiotics critical
– Extended antibiotic coverage sometimes
– Monitor closely post-operatively
Rehabilitation and Physical Therapy
Principles
Balance:
– Activity vs rest
– Exercise vs overuse
– Load management
Progression:
– Gradual increase in activity
– Respect pain and inflammation
– Modify during flares
Exercise Types
Range of Motion:
– Daily gentle ROM exercises
– Prevent contractures
– Maintain flexibility
Strengthening:
– Isometric exercises during flares
– Progressive resistance when stable
– Protect joints (avoid high impact)
– Focus on periarticular muscles
Cardiovascular:
– Low-impact activities (swimming, cycling, walking)
– Improve overall health
– Weight management
– Reduce cardiovascular risk
Functional:
– Activities of daily living practice
– Work-related tasks
– Sport-specific if appropriate
Occupational Therapy
Joint Protection:
– Ergonomic modifications
– Proper body mechanics
– Avoid positions of deformity
– Use larger, stronger joints
Adaptive Equipment:
– Assistive devices for ADLs
– Workplace modifications
– Home modifications
– Energy conservation techniques
Splinting:
– Rest splints (night)
– Functional splints (day)
– Serial splinting for contractures
Lifestyle Modifications
Diet and Nutrition
Anti-Inflammatory Diet:
– Mediterranean diet beneficial
– Omega-3 fatty acids (fish oil)
– Fruits and vegetables
– Whole grains
– Limit processed foods
Weight Management:
– Reduce joint stress
– Improve overall health
– May improve disease activity
Specific Considerations:
– Low purine diet for gout
– Calcium and vitamin D (osteoporosis risk)
– Folate supplementation (methotrexate)
Smoking Cessation
Critical:
– Smoking worsens RA
– Reduces treatment effectiveness
– Increases surgical complications
– Affects bone healing
Stress Management
Impact:
– Stress can trigger flares
– Affects pain perception
– Influences immune function
Techniques:
– Mindfulness and meditation
– Cognitive-behavioral therapy
– Support groups
– Counseling
Sleep
Importance:
– Adequate sleep essential
– Fatigue management
– Pain control at night
– Proper mattress and pillows
Prognosis and Long-Term Outlook
With Modern Treatment
Disease-Modifying Effect:
– DMARDs and biologics slow/stop progression
– Early aggressive treatment improves outcomes
– Remission achievable in many cases
– Functional outcomes much improved vs past
Factors Affecting Prognosis
Better Prognosis:
– Early diagnosis and treatment
– Good response to medications
– Medication compliance
– Healthy lifestyle
– No smoking
– Multidisciplinary care
Worse Prognosis:
– Delayed treatment
– High disease activity
– Positive RF and anti-CCP (RA)
– Multiple joint involvement
– Systemic manifestations
– Erosions at presentation
– Smoking
Long-Term Complications
Joint:
– Progressive damage if uncontrolled
– Need for multiple surgeries
– Functional limitations
Systemic:
– Cardiovascular disease (increased risk)
– Osteoporosis
– Infections (from treatment)
– Lung disease
– Eye complications
Monitoring
Regular Follow-Up:
– Rheumatology visits every 3-6 months
– Disease activity assessment
– Monitor for extra-articular manifestations
– Medication side effect monitoring
Laboratory:
– Inflammatory markers
– Complete blood count
– Liver and kidney function
– Lipids (cardiovascular risk)
Imaging:
– Periodic X-rays to assess progression
– MRI for specific concerns
Living with Inflammatory Arthritis
Self-Management
Education:
– Understand your condition
– Know your medications
– Recognize flares early
– When to seek help
Symptom Monitoring:
– Track disease activity
– Identify triggers
– Journal symptoms
Medication Adherence:
– Take as prescribed
– Don’t stop without consulting doctor
– Report side effects
Psychological Impact
Common Issues:
– Depression and anxiety
– Chronic pain
– Functional limitations
– Body image concerns
– Fear of future
Support:
– Mental health counseling
– Support groups (in-person or online)
– Family education and involvement
– Peer connections
Social and Work Considerations
Employment:
– Discuss needs with employer
– Workplace accommodations
– Disability considerations if needed
– Vocational rehabilitation
Relationships:
– Communication with family/friends
– Impact on intimacy
– Social activities modification
Planning for Flares
Recognize Early Signs:
– Increased pain
– More stiffness
– Swelling
– Fatigue
Management Plan:
– Increase rest
– Ice or heat
– Adjust activities
– Contact rheumatologist
– May need medication adjustment or injection
Emerging Treatments and Research
New Medications:
– Novel biologics
– Oral small molecule inhibitors
– Biosimilars (cost reduction)
Precision Medicine:
– Biomarkers to predict response
– Personalized treatment selection
– Early identification of aggressive disease
Regenerative Medicine:
– Stem cell therapies (experimental)
– Tissue engineering
– Cartilage restoration
Conclusion
Inflammatory arthritis encompasses a diverse group of conditions requiring comprehensive, multidisciplinary management. While these conditions can be challenging, modern medical treatments have revolutionized outcomes. Early diagnosis and aggressive treatment with DMARDs and biologics can prevent joint damage and maintain function. Orthopedic interventions play a crucial role when medical management alone is insufficient, offering pain relief and functional restoration. Success requires collaboration between rheumatology and orthopedics, combined with patient education, lifestyle modifications, and self-management. With appropriate treatment and monitoring, many patients with inflammatory arthritis can achieve remission or low disease activity and maintain an excellent quality of life. If you’re experiencing joint pain, stiffness, and swelling, especially with morning stiffness lasting more than 30-60 minutes, consult a rheumatologist promptly. Early intervention is key to the best outcomes.