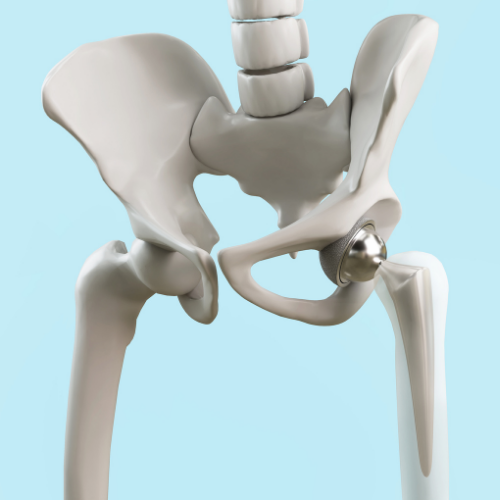
What is Hip Replacement?
Hip replacement, or total hip arthroplasty (THA), is a surgical procedure that involves removing damaged sections of the hip joint and replacing them with artificial components made of metal, ceramic, or plastic. It’s one of the most successful operations in orthopedic surgery, with excellent outcomes for pain relief and functional restoration.
Primary Indications for Hip Replacement
1. Osteoarthritis (Most Common)
Osteoarthritis is the leading indication for hip replacement, accounting for over 90% of cases.
Characteristics:
– Progressive wearing away of hip cartilage
– Bone-on-bone contact in advanced stages
– Age-related “wear and tear” arthritis
– Typically affects people over 50
When Surgery is Indicated:
– Severe pain interfering with daily activities
– Significant limitation in walking distance
– Pain at rest or during night
– Failed conservative management for 3-6 months
– X-ray evidence of joint space loss and bone changes
2. Rheumatoid Arthritis
An autoimmune inflammatory condition affecting the joint lining.
Key Features:
– Systemic inflammatory disease
– Often affects multiple joints
– Can occur at any age
– May involve younger patients than osteoarthritis
Surgical Indications:
– Persistent pain despite medical management
– Progressive joint destruction
– Significant functional impairment
– Disease affecting quality of life despite medications
3. Avascular Necrosis (Osteonecrosis)
Death of bone tissue due to insufficient blood supply to the femoral head.
Common Causes:
– Corticosteroid use (chronic or high-dose)
– Excessive alcohol consumption
– Trauma (hip fracture or dislocation)
– Sickle cell disease
– Caisson disease (decompression illness)
– Idiopathic (no identifiable cause)
When Replacement is Needed:
– Advanced collapse of the femoral head
– Severe pain limiting function
– Failed core decompression or bone grafting
– Involvement of the acetabulum (hip socket)
4. Post-Traumatic Arthritis
Arthritis developing after hip injury.
Typical Scenarios:
– Previous hip fracture
– Acetabular (hip socket) fracture
– Hip dislocation
– Prior hip surgery
Indications for Surgery:
– Progressive joint degeneration despite initial healing
– Chronic pain affecting daily life
– Mechanical symptoms (catching, locking)
– Failed joint preservation procedures
5. Hip Fractures
Particularly in elderly patients with specific fracture patterns.
Types Requiring Replacement:
– Displaced femoral neck fractures in elderly
– Failed internal fixation of hip fractures
– Pathological fractures through diseased bone
Patient Considerations:
– Age typically over 65-70
– Active lifestyle before fracture
– Medical fitness for surgery
– Desire to return to independent living
6. Developmental Dysplasia of the Hip (DDH)
Congenital hip abnormality leading to premature arthritis.
Characteristics:
– Shallow acetabulum (hip socket)
– Abnormal hip joint development
– Often diagnosed in childhood but may present in adults
– Leads to early-onset arthritis
Surgical Timing:
– When pain becomes significant
– Typically in 30s-50s age range
– Before severe bone deformity develops
– May require specialized implants and techniques
7. Ankylosing Spondylitis
Inflammatory arthritis affecting spine and potentially hips.
Hip Involvement Features:
– Stiffness and fusion of hip joint
– Bilateral hip involvement common
– Young to middle-aged males most affected
– Associated with spinal stiffness
Indications:
– Severe hip stiffness limiting mobility
– Pain affecting quality of life
– Failed medical management
– Functional disability
8. Septic Arthritis (Late Stage)
Joint infection leading to cartilage destruction.
Considerations:
– Must clear infection first (staged procedure)
– Complete destruction of joint surfaces
– Failed joint preservation
– Two-stage revision may be required
9. Bone Tumors
Benign or malignant tumors affecting the hip region.
Situations:
– Tumor removal requires joint excision
– Pathological fracture through tumor
– Giant cell tumor of proximal femur or acetabulum
– Metastatic disease causing bone destruction
10. Legg-Calvé-Perthes Disease (Late Sequelae)
Childhood condition affecting hip blood supply, leading to adult arthritis.
Long-term Effects:
– Deformed femoral head from childhood disease
– Early-onset arthritis in 30s-40s
– Often requires complex reconstruction
Clinical Criteria Beyond Diagnosis
Pain Assessment
Location:
– Groin pain (classic hip joint pain)
– Lateral hip pain
– Buttock or thigh pain
– Pain may radiate to knee
Severity Indicators:
– Pain with weight-bearing activities
– Start-up pain (pain when initiating movement)
– Night pain disrupting sleep
– Pain at rest in advanced cases
Functional Limitations
Activities of Daily Living:
– Difficulty putting on shoes and socks
– Trouble getting in/out of car
– Cannot walk more than 1-2 blocks
– Stairs become challenging
– Inability to perform work duties
Quality of Life Impact:
– Social isolation due to mobility issues
– Depression related to chronic pain
– Dependence on walking aids
– Limitation of recreational activities
Physical Examination Findings
Range of Motion:
– Significant restriction in hip rotation
– Limited flexion and extension
– Pain at end range of motion
– Positive impingement tests
Gait Abnormalities:
– Antalgic gait (limping to reduce pain)
– Trendelenburg gait (hip instability)
– Shortened stride length
– Use of assistive devices
Radiographic Evidence
X-ray Findings:
– Joint space narrowing or obliteration
– Subchondral sclerosis (bone hardening)
– Osteophyte formation (bone spurs)
– Subchondral cyst formation
– Femoral head deformity
Advanced Imaging:
– MRI for avascular necrosis detection
– CT scan for bone deformity assessment
– Bone scan for infection or tumor evaluation
Failed Conservative Treatment
Before considering hip replacement, patients should have attempted:
Non-Pharmacological:
– Physical therapy (3-6 months minimum)
– Weight loss if overweight
– Activity modification
– Assistive devices (cane, walker)
Pharmacological:
– NSAIDs or acetaminophen
– Corticosteroid injections
– Hyaluronic acid injections (less common in hip)
Other Interventions:
– Core decompression (for early AVN)
– Hip arthroscopy (for impingement or labral tears)
– Proximal femoral osteotomy (for dysplasia)
Special Populations
Young Patients (Under 50)
Considerations:
– Higher activity demands
– Longer life expectancy requiring revision
– Consider joint preservation procedures first
– Modern implants and techniques improving outcomes
Elderly Patients (Over 75)
Considerations:
– Medical comorbidities assessment
– Frailty evaluation
– Goals of surgery (pain relief vs high function)
– Risk-benefit analysis with anesthesia
Obese Patients
Considerations:
– Higher surgical risks
– Increased implant wear
– Wound healing concerns
– Should attempt weight loss first when possible
Absolute and Relative Contraindications
Absolute Contraindications:
– Active hip infection
– Sepsis or systemic infection
– Absent or insufficient bone stock
– Non-functional quadriceps or abductor muscles
– Severe peripheral vascular disease
Relative Contraindications:
– Morbid obesity (BMI > 40)
– Recent hip infection (within 1 year)
– Neurological disorders affecting hip control
– Poor skin condition around hip
– Mental health conditions limiting rehabilitation
– Active substance abuse
– Significant medical comorbidities
Making the Decision
Questions to Ask Your Surgeon:
- Have we exhausted all conservative options?
- What type of hip replacement approach do you recommend?
- What implant types and materials will be used?
- What are the expected outcomes and potential complications?
- What is your experience with hip replacement surgery?
- What does the recovery timeline look like?
- What are the activity restrictions after surgery?
- When might I need a revision surgery?
Shared Decision-Making Process:
– Discuss your goals and expectations
– Review your specific medical history
– Consider timing based on your life circumstances
– Understand the commitment to rehabilitation
– Get a second opinion if uncertain
Key Takeaways
– Hip replacement is indicated primarily for severe arthritis causing pain and functional limitation
– Multiple conditions can lead to hip replacement, with osteoarthritis being most common
– Conservative treatment should be attempted for 3-6 months in most cases
– The decision should be based on pain severity, functional impairment, and quality of life impact
– Patient-specific factors including age, activity level, and comorbidities influence surgical planning
– Modern hip replacement has excellent success rates with significant pain relief and functional improvement
Conclusion
Hip replacement is a proven, effective treatment for end-stage hip disease when conservative measures fail. The indications are clear: significant pain, functional impairment, radiographic evidence of joint damage, and failed non-operative treatment. If you’re experiencing these symptoms, consult with an orthopedic surgeon specializing in hip replacement to determine if you’re a candidate for this life-changing procedure.