Is Total Knee Replacement Necessary for You?
Total knee replacement (TKR), also known as total knee arthroplasty, is a surgical procedure that replaces damaged or diseased knee joint surfaces with artificial components. While it’s one of the most successful orthopedic procedures, it’s not always the first or only solution for knee problems.
When Conservative Treatment Isn’t Enough
Total knee replacement becomes necessary when:
– Chronic knee pain significantly interferes with daily activities like walking, climbing stairs, or getting in and out of chairs
– Pain persists even at rest or during the night
– Chronic inflammation and swelling that doesn’t improve with rest or medications
– Knee deformity causing visible bowing in or out of the knee
– Stiffness limiting the ability to bend or straighten the knee
– Conservative treatments have failed to provide adequate relief
Are You a Candidate for Total Knee Replacement?
Ideal Candidates Typically Have:
Medical Conditions:
– Advanced osteoarthritis (most common indication)
– Rheumatoid arthritis or other inflammatory arthritis
– Post-traumatic arthritis following knee injury
– Avascular necrosis (bone death due to insufficient blood supply)
– Severe knee deformities
Clinical Criteria:
– Age typically over 50 (though younger patients may qualify in severe cases)
– BMI preferably under 40 (obesity increases surgical risks and implant wear)
– Completion of at least 3-6 months of conservative treatment without success
– X-ray evidence showing severe joint space narrowing and bone-on-bone contact
– Realistic expectations about outcomes and recovery
Who May NOT Be a Good Candidate:
– Active infection in or around the knee
– Severe peripheral vascular disease
– Inadequately controlled diabetes
– Significant muscle weakness or paralysis around the knee
– Mental health conditions affecting rehabilitation compliance
– Young, highly active patients (increased risk of implant wear and need for revision)
– Morbid obesity (should consider weight loss first)
What Are Your Options?
Before committing to total knee replacement, consider these alternatives:
Non-Surgical Options:
Lifestyle Modifications:
– Weight loss to reduce joint stress
– Low-impact exercises (swimming, cycling, water aerobics)
– Activity modification to avoid aggravating movements
– Assistive devices (cane, walker, knee brace)
Physical Therapy:
– Strengthening exercises for quadriceps and hamstrings
– Range of motion exercises
– Balance and proprioception training
– Manual therapy techniques
Medications:
– NSAIDs (non-steroidal anti-inflammatory drugs)
– Acetaminophen for pain relief
– Topical analgesics
– Disease-modifying drugs for inflammatory arthritis
Injections:
– Corticosteroid injections for inflammation
– Hyaluronic acid (viscosupplementation) injections
– Platelet-rich plasma (PRP) – emerging therapy
– Stem cell therapy – still experimental for knee arthritis
Surgical Alternatives:
Arthroscopic Surgery:
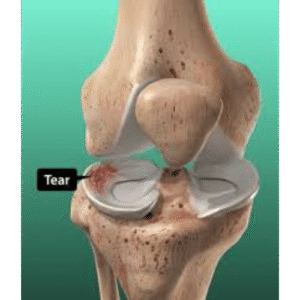
– Suitable for meniscal tears or loose bodies
– Limited benefit in advanced arthritis
– Minimally invasive with faster recovery
High Tibial Osteotomy:
– Realigns the leg to shift weight from damaged area
– Best for younger patients with single-compartment arthritis
– Preserves natural knee joint
Partial Knee Replacement (Unicompartmental):
– Replaces only the damaged compartment
– Smaller incision and faster recovery
– Preserves more bone and ligaments
– Not suitable for widespread arthritis
When Should You Get It Done?
Timing is crucial for optimal outcomes:
Right Time Indicators:
Quality of Life Impact:
– Pain prevents you from enjoying activities you love
– Sleep is regularly disrupted by knee pain
– You’re limiting social activities due to mobility issues
– Depression or anxiety related to chronic pain
Functional Limitations:
– Unable to walk more than a few blocks
– Difficulty performing job duties
– Struggling with basic self-care activities
– Relying heavily on pain medications
Medical Readiness:
– Overall health is optimized
– Chronic conditions are well-controlled
– You can commit to 3-6 months of rehabilitation
– You have adequate support at home for recovery
When to Wait:
– Conservative treatments haven’t been fully explored
– You’re planning significant weight loss
– Major life events are imminent (wedding, job change)
– Winter months if recovery at home would be challenging
– Infection or illness needs resolution first
Is Partial Knee Replacement an Option for Me?
Partial knee replacement (PKR) or unicompartmental knee arthroplasty can be an excellent option for select patients.
Ideal Candidates for Partial Knee Replacement:
Anatomical Requirements:
– Arthritis confined to one compartment (medial, lateral, or patellofemoral)
– Intact cruciate ligaments (especially ACL)
– No significant deformity (less than 10-15 degrees)
– Good range of motion
– Minimal to no inflammatory arthritis
Patient Characteristics:
– Age typically 55-75 years
– Normal to moderately overweight
– Active lifestyle but not extreme athletes
– Realistic expectations
Advantages of Partial Over Total:
– Smaller incision (3-4 inches vs 6-8 inches)
– Shorter hospital stay (often outpatient or 1 night)
– Faster recovery (return to activities in 4-6 weeks vs 3-4 months)
– More natural knee feel and kinematics
– Easier revision to total knee if needed later
– Less blood loss
– Lower risk of complications
Disadvantages to Consider:
– Not suitable if arthritis is widespread
– Slightly higher revision rate than total knee
– May eventually progress to total knee replacement
– Requires more precise surgical technique
– Limited long-term data compared to total knee
The Decision-Making Process:
1.Comprehensive Evaluation: Your surgeon will perform physical examination and review imaging
2.Discussion of Goals: Consider your activity level, expectations, and lifestyle
3.Risk-Benefit Analysis: Weigh surgical risks against potential benefits
4.Second Opinion: Don’t hesitate to seek another expert’s perspective
5.Shared Decision Making: This should be a collaborative choice between you and your surgeon
Key Takeaways
– Total knee replacement is highly successful but should be considered after conservative treatments fail
– Not everyone with knee arthritis needs surgery immediately
– Partial knee replacement offers advantages for patients with isolated compartment disease
– Timing matters—surgery should align with your quality of life, medical readiness, and functional needs
– Work closely with your orthopedic surgeon to determine the best approach for your specific situation
Next Steps
If you’re considering knee replacement:
1. Consult with a board-certified orthopedic surgeon specializing in knee surgery
2. Get appropriate imaging (X-rays, possibly MRI)
3. Explore all conservative treatment options thoroughly
4. Optimize your health before surgery
5. Understand the commitment required for successful rehabilitation
Remember, knee replacement is a life-changing procedure that can restore function and eliminate pain, but it requires careful consideration, proper patient selection, and dedication to recovery.